Food sensitivity tests (often sold as at‑home kits) measure IgG antibodies to foods, but experts warn they are not reliably accurate for diagnosing food intolerances. In simple terms, a high IgG level usually means you’ve eaten that food a lot, not that it’s causing harm. Major medical organizations (AAAI, the Canadian Society of Allergy & Clinical Immunology, etc.) explicitly advise against using IgG-based tests for sensitivities. In short: these tests work by checking your immune memory (IgG) against foods, but science shows IgG often reflects tolerance, not an allergy or intolerance. (For example, a person who eats wheat daily may have high wheat IgG simply from exposure, not because wheat is causing problems.)
How Food Sensitivity Tests Work (The Theory)
- Sample collection. You prick your finger (or sometimes send saliva/hair) and mail a small blood sample to a lab.
- IgG antibody analysis. The lab exposes your sample to a panel of food proteins (sometimes 100+ foods) and measures immunoglobulin G (IgG) levels for each.
- Result interpretation. Test reports list foods with “elevated IgG” as potential sensitivities or triggers. Kits typically advise you to eliminate those high‑IgG foods from your diet.
Proponents claim this finds hidden intolerances, but doctors caution the logic is flawed. IgG is the most common antibody and acts like an immune “memory.” Having IgG for a food usually means you’ve been exposed to it, not that it’s hurting you. In fact, experts note that IgG4 antibodies are often higher in people who tolerate foods well. For example, a baker will have high wheat IgG (from handling flour daily) even if they have no wheat symptoms.
IgG tests are not the same as allergy tests. True food allergies involve IgE antibodies and cause immediate, sometimes dangerous reactions (hives, breathing trouble). Food sensitivities/intolerances cause milder, delayed issues (bloating, headache, fatigue) and have no standard test. (Mayo Clinic experts emphasize there is no single validated test for food sensitivities.) At-home kits label IgG as a “sensitivity,” but science says IgG is not a proven marker of symptoms.
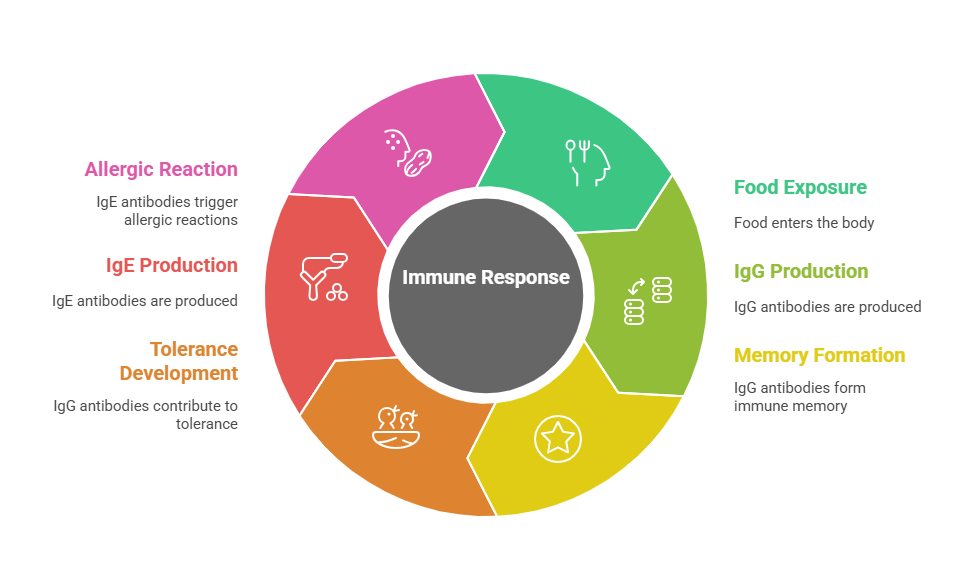
IgG vs. IgE – Allergy vs. Tolerance
It helps to know the difference: IgE antibodies cause true food allergies (peanuts, shellfish, etc.) – these reactions are often immediate and can be severe. IgG antibodies, on the other hand, appear hours or days later and are a normal part of our immune response. As Mayo Clinic explains: “An immunoglobulin G antibody is a memory antibody, and it determines exposure to a food – not an allergy… higher levels of IgG4 are associated with better tolerance to foods.”. In other words, IgG tells you you’ve seen the food before, not the food is hurting you.
Most medical labs and allergists do not use IgG testing. Instead, they focus on IgE tests and clinical history. An allergist might do a blood IgE panel or a skin-prick test if an allergy is suspected. For digestive intolerances (like lactose intolerance), doctors use enzyme tests or breath tests, not IgG panels. The bottom line: IgG tests are neither gold-standard nor FDA-approved for identifying food sensitivities.
Scientific Consensus: Why Accuracy Is Questioned
Experts agree: IgG food sensitivity tests lack scientific validation. Leading allergy organizations have publicly warned against them. The AAAAI flatly states such tests have “never been scientifically proven to accomplish what they report”. A Mayo Clinic Q&A notes “research does not support immunoglobulin G food sensitivity tests” and calls them misleading.
Healthline’s medical review echoes this: “Food sensitivity tests are not currently considered a reliable or accurate method of diagnosing food sensitivities,” and the AAAAI does not endorse home testing. Likewise, the Canadian Society of Allergy says IgG panels are unsupported. In fact, a 2022 Mayo Clinic response highlights that the lack of any valid test for “food sensitivities” is recognized by AAAAI, CSACI, and even the European allergy society.
Research also casts doubt on the premise. Dr. Sara May of Nebraska Medicine explains that blood IgG tends to be high for foods we eat often, not for foods that harm us. She warns many patients end up on needlessly restrictive diets after these tests. Similarly, Hackensack Meridian experts note “research has not shown that [IgG] tests are valid,” and that elevated IgG could come from an overactive immune system or infection – not a food reaction. A 2025 scientific review concluded that current guidelines discourage routine IgG testing, since these antibodies usually indicate exposure or inflammation, not allergy.
Putting it plainly: High IgG often just reflects that you eat a food. Many people (even healthy ones) have IgG antibodies to common foods. For example, studies showed bakery workers with high wheat IgG had no symptoms, and high IgG4 is actually linked to tolerance. Even if an IgG-guided diet helped someone feel better, critics argue it’s because the diet happened to cut out usual triggers (like wheat or dairy), not because the test “magically” identified them.
Why These Tests Can Be Misleading
Because of the above, IgG tests can easily mislead. Test reports often flag dozens of foods (the more you eat, the more “reactive” you appear), causing anxiety. Patients may think they’re sensitive to most of their diet. Mayo Clinic dietitians caution that these tests “can lead to unnecessary food restrictions, increased stress and anxiety around food, fear of foods, as well as overall poor nutrition”. In some cases, eliminating so many foods can even worsen gut symptoms or cause nutritional deficiencies.
In real life, the causes of chronic symptoms (bloating, headaches, fatigue) are often complex. An IgG test won’t catch them. For instance, one person might have gut symptoms from stress or IBS, and another might react to a food additive, hormone fluctuations, or an undiagnosed GI condition – things an IgG panel can’t pinpoint. Doctors warn that relying on these tests can delay the correct diagnosis. As Mayo experts advise, if you’re sick and curious about foods, it’s better to consult an allergist, gastroenterologist, or registered dietitian before trusting a home kit.
Better Approaches: Journals, Elimination Diets, and Professional Help
So what should you do if you suspect a food is causing trouble? Start simple: keep a food-symptom journal. Track what you eat and when symptoms occur. Over a few weeks, patterns often emerge on their own. If not, consider a supervised elimination diet: cut out the most common offenders (dairy, gluten, eggs, etc.) for a few weeks, then reintroduce them one at a time and watch your body’s response. Allergists and dietitians use this tried-and-true method because it directly tests your body’s reaction.
If an allergy is a concern (e.g. eczema, hives, asthma), professional IgE testing (skin or blood) is appropriate. For gut-specific issues like lactose or fructose intolerance, doctors have specific tests (breath tests, stool studies) that are validated. And, very importantly: work with a professional. A doctor or dietitian can help ensure you don’t cut out too many foods and miss essential nutrients. They can order proper tests when needed and interpret results in context.
Bottom Line
In a nutshell, most experts advise against at-home IgG food sensitivity tests as a diagnostic tool. They measure your immune “memory” (IgG) to foods, which usually signals tolerance or past exposure, not true intolerance. Clinical experience and guidelines are clear: these tests aren’t proven and often cause more confusion than help. If you have unexplained symptoms, focus on careful monitoring of your diet and symptoms, consider an elimination diet, and seek medical guidance. That approach may take more time and patience, but it’s far more likely to pinpoint real triggers safely than an unproven home test. If you want personalized support and professional interpretation, you can explore our food sensitivity testing service page.


