A trigger point injection targets a tight, painful “knot” in a muscle called a trigger point that isn’t releasing on its own. The injection delivers a local anesthetic (and sometimes a corticosteroid) directly into the knot, which relaxes the contracted muscle fibers, blocks pain signals, reduces local inflammation, and restores normal blood flow to the area. Relief typically begins within 24 to 72 hours and can last weeks to months, depending on the person and the condition being treated.
If you’ve ever had a persistent muscle knot that a massage couldn’t budge, a stretch couldn’t reach, and rest didn’t fix — you already understand the frustration that brings most people to ask about trigger point injections. The pain is specific, sometimes radiating, and often stubborn in a way that makes conservative treatments feel useless.
Trigger point injections are not a new procedure. They’ve been used in pain management and rehabilitation medicine for decades. But there’s still a lot of confusion about exactly how they work, what they’re best for, and what a realistic outcome looks like. This guide answers those questions clearly, without the medical jargon.
What Is a Trigger Point, Exactly?
Before understanding what the injection does, it helps to understand what it’s targeting.
A trigger point is a hyperirritable spot within a taut band of skeletal muscle. In plain terms: it’s a localized area where muscle fibers have contracted and aren’t releasing. The muscle isn’t just “tight” it’s stuck in a sustained contraction at the fiber level, which disrupts blood flow, causes metabolic waste to accumulate, and sensitizes the local nerve endings.
What makes trigger points distinct from general muscle soreness is their behavior. They often cause referred pain — pain felt in a different location from where the knot actually is. A trigger point in your shoulder, for example, can produce a headache at the base of your skull. A knot in your hip flexors can mimic lower back pain. This pattern of referred pain was first systematically documented by physicians Janet Travell and David Simons, whose work in the 1950s through 1990s laid the foundation for modern trigger point therapy.
| Active trigger points | Latent trigger points |
| Painful even without being touched Produce referred pain patterns Often cause restricted range of motion Can disrupt sleep and daily function | Only painful when pressed Tightness without spontaneous pain Can become active with stress, overuse, or injury May cause muscle weakness or stiffness |
What Does a Trigger Point Injection Actually Do?
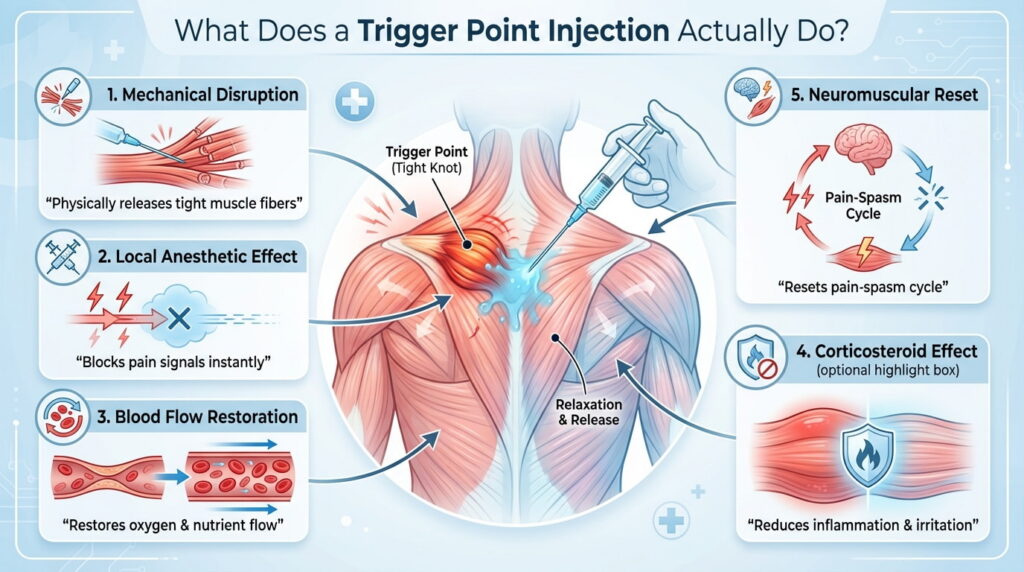
This is the question most people really want answered. The injection works through a combination of mechanical and chemical effects that together interrupt what’s called the “pain-spasm cycle” — the loop where pain causes muscle contraction, contraction causes more pain, and so on.
Here’s what happens at each level:
- Mechanical disruption of the knot: The physical act of the needle entering the muscle tissue helps break up the contracted fibers. The needle disrupts the tight band mechanically, allowing the fibers to release from their sustained contraction. Some providers use a peppering technique – redirecting the needle in multiple directions from a single entry point – to maximize disruption of the trigger point band.
- Local anesthetic: blocking the pain signal: Most trigger point injections use a local anesthetic such as lidocaine or bupivacaine. The anesthetic floods the local tissue and blocks the nerve receptors in the area, interrupting pain signal transmission almost immediately. This is why many patients feel significant relief within minutes of the injection. As the anesthetic wears off over a few hours, the underlying muscle may ache temporarily before longer-term relief sets in.
- Improved blood flow and waste clearance: A sustained muscle contraction cuts off normal blood circulation to the affected area. Without adequate blood flow, the muscle cannot get enough oxygen, and metabolic waste products – including lactic acid and inflammatory compounds – accumulate. The injection restores normal circulation: fresh oxygenated blood flows in, and waste products are carried away.
- Corticosteroids: Some trigger point injections include a corticosteroid such as methylprednisolone or triamcinolone, particularly when significant inflammation is present. The steroid reduces local tissue inflammation, calms sensitized nerve endings, and can extend the duration of pain relief. Not all injections include a steroid – it depends on the clinical picture.
- Resetting the neuromuscular circuit: Beyond the immediate mechanical and chemical effects, trigger point injections appear to influence how the central nervous system processes pain signals from that region. Breaking the local pain cycle can reset sensitized pain pathways, reducing central sensitization and allowing the nervous system to normalize its response.
What to Expect: Before, During, and After
Most people who are considering trigger point injections have two main concerns: does it hurt, and does it actually work? Both are reasonable. Here’s an honest walk-through of the experience.
Before the injection
Your provider will take a history of your pain when it started, what makes it better or worse, what treatments you’ve already tried, and whether you have any relevant medical conditions or allergies (particularly to local anesthetics). They’ll then palpate the muscle by hand, pressing firmly along the suspected trigger point area to identify the exact location of the knot and reproduce your familiar pain. Finding that “yes, that’s it” spot is central to accurate injection placement.
You may be asked to avoid taking blood thinners like aspirin or ibuprofen for a day or two beforehand, and to wear clothing that allows easy access to the injection site.
During the injection
The area is cleaned with an antiseptic. A thin needle typically a short, fine gauge needle is inserted directly into the trigger point. Most patients report one of two sensations at this moment:
- A sharp pressure or aching sensation as the needle enters the taut muscle band.
- A brief involuntary muscle twitch or spasm, called a local twitch response — this is actually a positive sign that the trigger point has been accurately located.
The twitch response can be startling if you’re not expecting it, but it’s brief and is generally considered confirmation that the needle has found its target. The anesthetic is then injected, and the needle is withdrawn. The entire procedure from needle insertion to withdrawal typically takes under a minute per injection site, though a session may involve multiple sites.
After the injection
Immediately after, the area may feel numb or tender. Some people experience a temporary increase in soreness called post-injection soreness that can last 1 to 3 days. This is normal and doesn’t mean the injection failed. A warm compress and light movement can help ease this soreness.
Pain relief typically begins within 24 to 72 hours as the anesthetic metabolizes, the muscle releases, and inflammation subsides. For some patients, relief begins almost immediately. For others, it takes a few days. How long relief lasts varies considerably:
| Relief duration | Who this typically applies to |
| Days to 2 weeks | Acute or newly developed trigger points; very sensitive individuals; first injection in a series |
| 2–6 weeks | Most common duration for a single injection in moderate myofascial pain |
| 1–3 months or longer | Well-established trigger points that respond well; patients who also do physical therapy between sessions |
| Long-term resolution | Possible when injections are combined with corrective exercise, posture work, and addressing root causes |
What Are the Risks and Side Effects?
Trigger point injections are generally considered safe when performed by a trained clinician. Serious complications are rare. That said, it’s important to go into any medical procedure with clear expectations about what can go wrong.
- Post-injection soreness – very common, usually resolves within 1–3 days; not a sign of failure
- Bruising or minor bleeding at the injection site – common and self-resolving.
- Temporary numbness or weakness from the local anesthetic – resolves as the anesthetic wears off.
- Infection – rare when proper sterile technique is followed.
- Pneumothorax (collapsed lung) – extremely rare, but a known risk for injections near the chest wall if technique is improper; another reason this must be done by a qualified clinician.
- Allergic reaction to the anesthetic or steroid – uncommon but possible; tell your provider about any known drug allergies.
- Atrophy or skin depigmentation at the site – rare, associated with frequent repeated steroid injections in the same location.
Trigger Point Injections at Lumē Wellness in Peoria, AZ
At Lumē Wellness, trigger point injections are offered as part of our comprehensive pain therapy approach. We don’t treat trigger point injections as a standalone fix, we evaluate each patient’s pain pattern, history, and contributing factors to understand why the trigger points developed in the first place.


